The new obesity drugs work, but it's a dilemma when people have to stop taking them
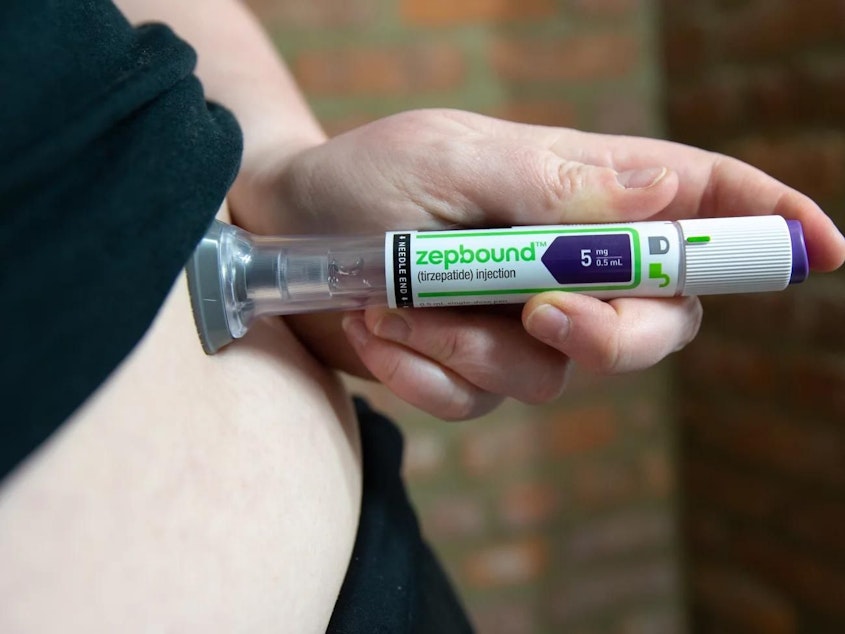
Over the past few decades, Jonathan Meyers endured several cycles of gaining, shedding, then regaining weight after attempting Keto, high protein, low fat, and calorie-restrictive diets. “I’ve had success, up and down, but I always regain the weight,” says Meyers, a digital strategist at an environmental nonprofit.
But on Zepbound – the newest GLP-1 agonistdrug to launch – Meyers lost 35 pounds and loves feeling free from hunger. Without what he calls “food noise” – the gnawing compulsion to eat – he consumes less and moves more.
But the drug’s been in short supply and very hard to find. Meyers even had family in Maine ship medicine in cold containers to him in Kensington, Maryland. Now, he can’t find Zepbound anywhere, and says friends, family, and people he follows on social media are all in the same boat. Some, he says, have turned to compound pharmacies selling approximations of the drug online; others tapered their doses, stretching them out.
More and more people who started taking the new GLP-1 agonist drugs are now confronting the realities of their limitations; medications like Wegovy and Mounjaro tend to help with sustained weight loss only while people are on them. But because of cost, for example, negative side effects, or supply shortages, many people are having to transition off of them — while trying not to regain the weight.
For many people, like Meyers, facing that resurfaces familiar anxieties about past failures relying on diet and exercise alone.
Sponsored
Meyers says before going on the injections, he felt his hungry impulses always won out in the end. “That's the biggest component of this whole thing,” he says. On the drug, he says he’s no longer preoccupied by food, and can walk past candy bars in the grocery store without grabbing one.
But he isn’t confident he could keep those distracting thoughts at bay in the long run, without pharmacological support.
And so far, clinical data seem to back up Meyers’ suspicions. One early study showed patients regained two-thirdsof the weight lost within the first year of stopping. New analysis showed 17% of people able to maintain 80% of their weight loss after stopping. And while experts say lifestyle choices like food and activity must be the cornerstone of all lasting weight loss plans, they also recognize those changes alone are often not enough for patients with obesity.
In other words: Chronic disease requires chronic treatment, no different than kidney disease, or high cholesterol. The new obesity treatments act on the various hormonal and metabolic drivers of obesity.
“It would make sense that once we stop the therapy for those biological problems, that we would have relapse,” says Dr. Eduardo Grunvald, director of the weight-management program at the University of California San Diego. He notes only the exceptional one or two of his patients have stopped the injections and not seen appetite and weight return.
Sponsored
But these are not just blockbuster medicines – they’ve become a societal phenomenon. And all the chatter about the use of them on social media and in popular culture can confuse patients, says Dr. Rekha Kumar, an endocrinologist and former medical director of the American Board of Obesity Medicine. She says social media is full of posts by people claiming to use obesity meds short term, as a kickstart to a diet saying, “‘Oh, I’m just going to take these for a short time and then stop.’”
But Kumar says these drugs were intended for medical use to treat the disease of obesity, not used to aid in cosmetic weight-loss. “Many of these people that we're hearing that from, don't actually qualify for the strict criteria of the medicine,” she says.
A person’s response to being on the drug — or to halting it — will depend on the particulars of their biology, genetics, or hormonal makeup. But for the vast majority of people, she says, biology favors regain. “We as humans – it’s evolutionary to want to store this fat and want to keep it on.”
That potential for weight regain is a major deterrent with these medicines. A poll from the health research organization KFF last year found only 14% of peopleremained interested in treatment, after hearing that weight tends to return after stopping.
Drug makers are already chasing longer-acting maintenance drugs.
Sponsored
In the meantime, Kumar says for those on them long term, transitioning on and off the drugs will be a reality many patients will face, if nothing else, because of other medical situations they may run into, such as a surgery or pregnancy. (To date, research on pregnant women and GLP1 medications suggest it is not linked to more birth defects than insulin, but the full impact of fetal exposure is not yet known. Women who have struggled with infertility are reporting surprise pregnancies after using GLP1 medicines, and the drug companies warn that they may make birth control pills less effective.)
“So there are going to be scenarios, especially in young people, [where] we will have to come off the medicine, whether they like it or not,” Kumar says.
What should patients faced with that situation do?
Obesity specialists recommend developing personalized plans with a doctor — tapering off the drugs, for example, while stepping up dietary counseling.
But there are also a lot of emotional changes to prepare for, too, says Dr. Natalie Muth, a pediatrician, obesity specialist and spokesperson for the American Academy of Pediatrics.
Sponsored
Many of her young patients who’ve taken the drug feel more hope, along with increased mobility and a sense of control. So when some of her patients encountered shortages recently, they also contended with a great deal of anxiety. “They felt it, they missed it, they were really distressed about it,” Muth says. She worked with the patients and their families to refocus on behavioral changes to manage their obesity as they transitioned off of them.
Jonathan Meyers, the Maryland man searching for Zepbound, has plenty of experience with the kind of drastic lifestyle changes necessary for him to lose weight without medication. It requires diligently tracking every bite, by scanning everything he eats into a mobile app, and limiting himself to about 1,000 calories a day, just enough to leave him ”just absolutely starving all the time.”
Instead, Meyers last month opted to buy the similar drugs sold by a compound pharmacy in Florida. He did so with his doctor’s cautious blessing and despite the various unknowns — like what’s in the drug, exactly, or how he might react to it.
After two weeks on the substitute, it’s a mixed bag, he says. He feels dyspeptic on it, but also hungrier. “It’s kind of like, ‘Oh, I want a little bit more,’ and it’s a little hard to push the plate aside.”
There’s also plenty of other uncertainties — about the short supply, fluctuating cost, and their long-term effects – but he says even those hassles are worth it. “To me, if I have GI problems for the rest of my life, but I don't have a heart attack or don't have all the other things associated with obesity, it's fine.”



